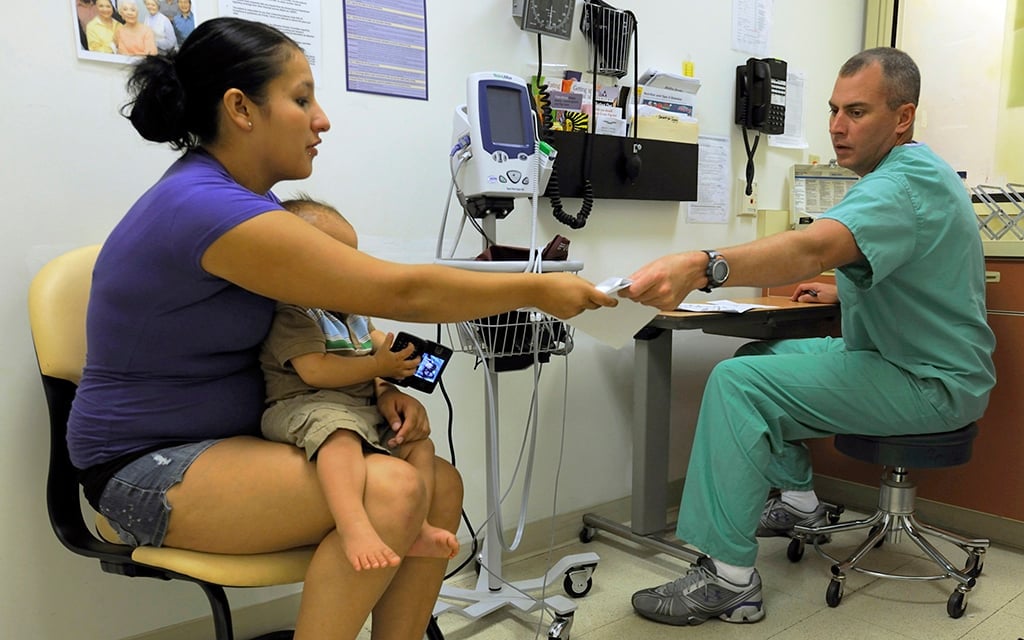
After being paused nationwide during the pandemic, states again began reviewing Medicaid recipients’ eligibility last year. It’s led to sharp enrollment drops across the country, but advocates say Arizona has handled the “unwinding” well. While enrollment has dropped, it’s still higher than before the pandemic. (Photo by Capt. Geoff Legler/Oklahoma Army National Guard)
PHOENIX – One year after restarting the pre-pandemic review process for enrollment in Medicaid and the Children’s Health Insurance Program, the Arizona Health Care Cost Containment System cut coverage for 611,144 recipients and approved 1,953,301 renewals, according to its eligibility dashboard. The agency is continuing to review coverage for 1,892 recipients as of April 5. The nationwide review process, referred to as “unwinding,” cut the Medicaid rolls in every state.
State agencies, like AHCCCS, go through a process every year known as “renewal and discontinuance.” During this process, recipients’ income levels are evaluated to determine if they still qualify for coverage through Medicaid or CHIP – the Children’s Health Insurance Program. However, during the COVID-19 pandemic, the Families First Coronavirus Response Act instructed states to suspend disenrollment efforts and extend coverage through March 2023.

Matt Jewett, director of health policy for the Children’s Action Alliance. (Photo courtesy of Children’s Action Alliance)
During this time Medicaid and CHIP enrollment grew to 92.3 million nationwide, an increase of over 20 million since the beginning of 2020. In Arizona, enrollment grew from 1.9 million to 2.5 million during the pandemic, according to Matt Jewett, director of health policy for the Children’s Action Alliance. Despite the unwinding process, over 2.2 million Arizonans still have full or partial coverage through Medicaid or CHIP, around 300,000 more than before the pandemic, as reported in the April 2024 AHCCCS Population Highlights report.
“We’re happy that the total number of people enrolled is still above what it was before the pandemic started,” Jewett said.
According to Medicaid, the expiration of continuous enrollment that happened during the pandemic is the “single largest health coverage transition since the first open enrollment period for the Affordable Care Act.”
AHCCCS, the Arizona agency in charge of Medicaid, reviewed medical criteria and ran 2.5 million Arizonans enrolled in Medicaid through the federal database and income sources to determine eligibility. Medicaid recipients received letters explaining the start of this process and their status, no matter if they were declared eligible or not.
“There are a lot of people who fell off; many of them managed to get back on,” said Jewett. “We don’t understand why some of those people lost coverage to begin with. Maybe they did not return their renewal forms on time, or they didn’t take action, or it could be some sort of technical or administrative glitches. But it sounds like AHCCCS is doing better than other states.”

Claudia Maldonado, director of outreach and enrollment at the Arizona Alliance for Community Health Centers. (Photo courtesy of the Arizona Alliance for Community Health Centers)
Those who weren’t automatically declared eligible or ineligible through the database were informed of their status through email and mail notifications sent out by AHCCCS. It told people to review their information for possible errors and verify that they exceeded the Medicaid income limit. Heidi Capriotti, communication administrator for AHCCCS, noted that a main reason for disenrollment was a lack of response from the Medicaid recipient.
For many recipients, this was their first experience with the review process, according to Claudia Maldonado, director of outreach and enrollment at the Arizona Alliance for Community Health Centers. Joint communication and outreach from state and local organizations was implemented to help guide recipients through the process.
“Those that did have to interact often went to maybe a community health center because they knew somebody there who could help them, as all of our health centers have people who are dedicated to helping people with their enrollment and questions and what have you,” Maldonado said.
Arizona’s average automatic renewal rate was 72% throughout the unwinding process that started in April 2023. AHCCCS got information through Equifax, the Department of Motor Vehicles, Medicare, the Social Security Administration and other sources to automatically verify eligibility and avoid staff intervention.
According to the Georgetown University Center for Children and Families, Arizona has the second highest “ex parte,” automatic renewal rate, in the country. This means that many Medicaid and CHIP recipients went through the renewal process without providing back-and-forth documentation because the AHCCCS was already in possession of necessary documents.

Jennifer Burns, senior director of legislative affairs at the Arizona Alliance for Community Health Centers. (Photo courtesy of the Arizona Alliance for Community Health Centers)
“We are one of the highest in the country,” said Jennifer Burns, senior director of legislative affairs at the Arizona Alliance for Community Health Centers. “It’s been very rewarding to see how well that went.” Burns attributed Arizona’s success to the collaboration between the various state agencies, managed care organizations, community health centers and the community at large.
Licensed navigators received lists of those who lost coverage and were available to help those people find coverage through the Affordable Care Act marketplace. Maldonado said navigators prioritized community outreach at school-based community resource centers, fairs and food banks where they understood the demographics of community members and their needs.
Meanwhile, community health centers worked with health plans like Medicaid to further localize outreach. Maldonado, at AACHC, participated in media coverage of the unwinding process on Spanish-language news and radio.
“Every community is different and has its own personality,” Maldonado said. “Some of our communities prefer radio and television over social media. So it’s understanding those nuances in our communities and then choosing those avenues that we know the messaging will have the greatest impact.”
After “unwinding” Medicaid for the first time in years, state and federal agencies will soon begin the review process for the coming year.

