PHOENIX – Twelve years ago, while pregnant with her second child, Shawn Soumilas began having contractions and thought she was in labor. But the pain was excruciating, and she knew something wasn’t right.
“I called my doctor, and she said, ‘Let’s go ahead and head over to the OB-GYN triage unit.’”
It was the day before the Fourth of July, and the hospital in Scottsdale was busy. Then a shift change occurred. A new nurse was supposed to perform a biophysical profile on the baby, checking for heart rate, breathing and movement, but, Soumilas said, she neglected to do so.
“I was a pebble under her shoe,” Soumilas recalled. “She just kept barking at me that I was dehydrated because it’s July in Scottsdale.”
Things quickly went downhill. Hospital personnel sent Soumilas for an ultrasound, but then the tech told her they needed her back in triage – without saying why. While waiting to be transported, Soumilas was overcome with nausea.
“My husband told me later, that’s when he felt like I was starting to die.”
Back in triage, Soumilas was met by a wall of doctors yelling, “Is that her? Is that her?”
They rushed her into an operating room and inserted an IV. Before she went completely dark, Soumilas remembers screaming, “Please, take care of my baby.”
When she awoke the next day, she asked her nurse, “Where’s my baby?” But she didn’t need to wait for a response to realize the worst had happened.
“I could tell by her eyes that he was gone.”
Counting kicks, helping moms
Soumilas later learned she had experienced a rare complication called a placental abruption, in which the placenta separates from the uterine wall before birth – sometimes depriving oxygen to an unborn child and causing internal bleeding in the mother.
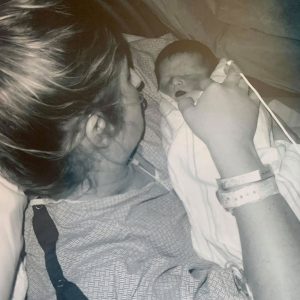
Shawn Soumilas is shown with her son, Zachary, in the hospital. Remembrance photos are sometimes taken for parents after the death of an infant. (Photo courtesy of Shawn Soumilas)
“I lost three times my blood volume,” she recalled, “and I needed blood, plasma and platelet transfusions. They told my husband I had about a 30% chance of getting through the surgery.”
By the time doctors got to the baby, he had been without oxygen for too long. Soumilas lost her son, Zachary, at 38 weeks.
As she recovered, Soumilas began researching everything she could about stillbirth, and one thing struck her. A symptom of placental abruption is decreased fetal movement, and two days before losing her baby, she’d reported to doctors that she hadn’t felt much movement.
“I was told lay on my side, drink some juice, see if he perks up. So I did that,” she said. “I was told, ‘His due date’s almost here; he’s probably settling down for birth.’ And that doesn’t happen. They don’t stop moving.
“If I would have been … tracking his patterns, then I would have known something had changed. If I would have gone in two days before, he would have been alive.”
Soumilas eventually discovered a campaign called Count the Kicks, dedicated to teaching expectant mothers about fetal movement and tracking the health of their unborn children. The effort grew out of the nonprofit Healthy Birth Day, started in 2008 in Iowa by five mothers who all lost daughters to stillbirth or infant death.
Working with state health agencies, the organization provides a free app or paper chart to help expectant mothers track their babies’ movements during the third trimester so that if they detect any unexpected changes, they can seek help immediately.
The campaign, already in 14 states, is expanding this month to Arizona. The Arizona Department of Health Services is partnering with Count the Kicks to get educational materials in multiple languages to health providers, birthing centers and others who are part of an expectant mom’s journey.
“Too many people think that stillbirth can’t be prevented. We strongly disagree,” said Emily Price, executive director of Count the Kicks. In 2010, Price noticed her baby’s movements had slowed, but because she had been tracking them, she alerted her doctor and her son, Hayden, was born healthy.
Stillbirth is the death of a fetus at 20 or more weeks during pregnancy. Causes may include infections, birth defects, lifestyle, or problems with the umbilical cord or placenta, as Soumilas experienced.
Stillbirths have decreased in the U.S. over the past 15 years. Nevertheless, nearly 22,000 were recorded in 2019, according to data from the Centers for Disease Control and Prevention.
Mothers most at risk include Black women, those 35 and older, women who smoke during pregnancy and those with such medical conditions as diabetes and obesity. But they aren’t alone.
“Hispanic women are at greater risk,” Price said. “Indigenous women are at greater risk. And it is completely unacceptable that in 2022, we are losing babies to stillbirth at the rate that we are.”
New research also shows that women sick with COVID-19 at the time of delivery face greater risk of stillbirth. One CDC study found that among 1,249,634 deliveries in March 2020 through September 2021, stillbirths occurred in 0.65% of deliveries. But among those with COVID-19 at the time of delivery, the stillbirth rate was 1.26%.
Arizona recorded nearly 500 stillbirths in 2019, the latest data available, with clear disparities among women of color.
“It’s a much larger problem in American Indian communities, as well as African American communities,” said Angie Lorenzo, who heads the office of women’s health at the state Department of Health Services. “Those are the two largest hit by this.”
Experts examining such disparities note that in many cases, a cause of death isn’t even documented, but they point to aggravating factors that include access to good health care, institutional bias and differences in health care before and during pregnancy.
“Racial disparities definitely persist,” said Stephaney Moody, health equity coordinator at Count the Kicks. “We’re not having the conversations. It’s not an easy one to have, but it’s one that I’m not afraid of doing.”
Warning signs – and solutions
Although lack of fetal movement is one warning sign of potential problems, experts disagree on whether counting kicks directly correlates to any decrease in stillbirths.
A 2009 study in the journal BMC Pregnancy Childbirth that reviewed previous research on fetal movement monitoring found some evidence of impact on stillbirths in high-risk pregnancies, but it recommended more study be done to determine the effect of universal fetal movement monitoring.
Another review in 2021 agreed that more study is necessary to evaluate the effectiveness of various methods of monitoring fetal movement, but it noted that “fetal movement count monitoring is a low-cost and low-tech method that has the potential to prevent worsening problems with unborn babies and merits the attention of providers and pregnant women.”
Count the Kicks is undertaking its own research as well. Researchers at Des Moines University and the Harkin Institute for Public Policy & Citizen Engagement surveyed 809 women who used the Count the Kicks app and determined that users increased their knowledge of movement patterns and were more likely to be seen by a doctor for decreased fetal movement.
The app that Count the Kicks developed works with expectant moms to track how long it takes to feel 10 movements, including kicking and rolling. Count the Kicks has also developed a paper form to track movements and average them out.
“Every baby and every pregnancy is different,” Moody said. “Maybe it would take my baby 10 minutes to get the 10 kicks… but it takes your baby 45 minutes. The key is knowing what is ‘normal.’”
In Arizona, the health department and Count the Kicks are working to specifically target underserved communities and women of color. Materials are available in English and Spanish, and Moody and Lorenzo said the goal is to provide brochures, posters and app reminder cards in Navajo as well.
The Department of Health Services is partnering with Diné College on the Navajo Nation and South Phoenix Healthy Start, a provider to women of color, to help spread word of the effort.
Moody said she hopes to see a drop in stillbirths in the state by introducing the program to “not only expecting parents, but also to the maternal health workers and providers that are in the state.”

Shawn Soumilas – along with her husband, Theo, and son, Ian – lights a candle at a vigil for parents grieving the death of a child. Soumilas now works with the group Count the Kicks to teach expectant mothers about fetal movement and tracking the health of their unborn children. (Photo courtesy of Shawn Soumilas)
Honoring Zach
After volunteering with Count the Kicks, Soumilas now represents Arizona as an ambassador for the organization – to share her story and spread awareness of the campaign. She connects with groups and hospitals that treat pregnant women, and is heartened that the partnership with AZDHS will bring added attention.
Today, Soumilas, 48, lives in Prescott with her husband, Theo, and 13-year-old son, Ian. But Zach is always in her heart.
“It will always be hard to know that Zach is supposed to be right by Ian’s side during all of our memorable family moments,” she said. “When I was pregnant with Zach, I felt a sense of peace that they would always have each other in life.”
And every day, she works to honor her son through her work with Count the Kicks.
“If you do see a change, you’ve got to speak up… Don’t wait until tomorrow,” she said. “Having that conversation is extremely important for women to know that you’re the one that’s empowered to do this for you.”




