
Lynn Metz and Artie Evans, who work for the Catholic aid organization Casa de Clara in San Jose, California, load a truck with food for homeless people on April 22. Monetary donations since the pandemic have afforded the organization the flexibility to buy food and other necessities. (Photo courtesy of Casa de Clara)
When the Downtown Emergency Service Center in Seattle moved its homeless residents from crowded shelters into hotels, staff worried about how to keep them connected to services. They decided to buy cellphones, tablets and laptops, and now their clients at the Red Lion Hotel can virtually attend medical appointments and meet with mental health specialists with greater flexibility than before the pandemic.
In San Francisco, homeless workers are providing small amounts of alcohol and nicotine to homeless people with addictions to encourage them to remain in quarantine. And throughout the country, shelter operators are seeing new life in people who have been relocated to hotels and motels that have been empty because of COVID-19 travel restrictions.
Emergency measures put in place to care for homeless people during the pandemic have turned into a roadmap for better services, such as medical care, addiction treatment and housing. Experts say these work-arounds suggest opportunities for new solutions to age-old problems faced by homeless people, and they could lead to a shift in funding and resources for homeless initiatives.
“Never let a crisis go to waste,” said Dr. Margot Kushel, a nationally recognized homelessness expert at the University of California, San Francisco. “I mean, we might as well take any silver lining we can.”
Health care from anywhere
Since the start of the pandemic in March, experts have worried how homeless people would receive the ongoing medical and behavioral health support many of them depend on, particularly those moved to temporary and emergency housing.
“For some people, being isolated, especially with mental illness, can be really, really frightening and scary,” said Bobby Watts, chief executive officer of the National Health Care for the Homeless Council. “You have to provide the support. And telehealth is a big way to do that in the time of COVID.”
A Harvard Medical School study suggests that about a quarter to a third of all homeless people have a serious mental illness, such as schizophrenia, bipolar disorder or severe depression. The flexibility of telehealth has allowed homeless people to keep their appointments with providers, something they struggled to do with in-person visits, Jannatul Ferdous, director of Behavioral Health at Health Care for the Homeless in Baltimore, said in a May 8 webinar on telehealth services hosted by the National Health Care for the Homeless Council.
After Seattle’s Downtown Emergency Service Center spent about $12,000 on digital devices and service plans to help staff and clients communicate virtually with health care providers, residents with mental illnesses, substance abuse disorders and chronic health conditions seemed to do better, said Noah Fay, the nonprofit’s director of housing.
“The clients have been amenable to it. The providers have been amenable to it. And I think that is a lesson that we would not have learned without this COVID situation,” said Daniel Malone, the center’s executive director. “I would have told you that there’s no way that telemedicine is remotely applicable to our circumstance and our clients. And it turns out that at least for some of them, there is a way to do it. And we’re really pleased to have learned that.”

Annie Valenciano of the Downtown Emergency Service Center in Seattle checks a homeless client in 2019. In response to the pandemic, the organization spent nearly $12,000 on smartphones, tablets and laptops so clients could access telehealth services while adhering to shelter-in-place mandates. (Photo courtesy of Downtown Emergency Service Center)
Watts said the biggest challenge was getting reimbursement. The U.S. Department of Health and Human Services is providing flexibility during the COVID-19 crisis for health care providers to waive or reduce costs for patients on Medicare. Before, Medicare would pay for only limited telehealth services.
The Centers for Medicare and Medicaid Services also broadened the range of practitioners who can bill through Medicare telehealth services to include physical therapists, occupational therapists and speech language pathologists.
One change of particular benefit to homeless people was the clearance to use audio-only telehealth, Watts said. In the past, reimbursement for telehealth had to include both audio and video, but the government lifted that requirement during the pandemic for behavioral health counseling, annual wellness visits, advance care planning, tobacco and smoking cessation counseling, and patient education services.
Many unhoused people have cellphones, but they don’t necessarily have smartphones, Dr. Regina Olasin, chief medical officer at Care for the Homeless in New York, said in the webinar. And even if they have a smartphone, Watts said, they may struggle to pay for data plans, which could prevent them from accessing health care.
The ability to talk by phone also increases the likelihood that people suffering from depression or anxiety will keep their appointments. If someone has a bad day, instead of canceling or not showing up, they can keep the appointment by phone, Marte McNally, behavioral health director at Nasson Health Care in Springvale, Maine, said during the webinar.
Lowering barriers to addiction treatment
The pandemic also is making addiction treatment more accessible, changes that Dr. Kimberly Sue, medical director of the nonprofit Harm Reduction Coalition in Oakland, California, called “absolutely necessary.”
Homeless people face disproportionately high rates of substance abuse, and in one Boston study published in the Journal of the American Medical Association, drug overdose was the leading cause of death among that population. Without stable housing or accessible addiction services, experts say, these individuals have significant difficulty following treatment plans.
In New York City, the Department of Health and Mental Hygiene lowered restrictions on methadone, a drug used to treat opioid addiction, allowing it to be delivered to homeless isolation sites, said Dr. Kelly Doran, assistant professor at New York University’s Grossman School of Medicine. Previously, people had to travel each day to methadone clinics, which required public transit and long waits in spaces that often were crowded.
“And so this is the sort of innovation that we’ve seen during COVID-19 that has been positive and has the potential to be particularly positive for groups like people experiencing homelessness,” Doran told the Howard Center for Investigative Journalism.
Amid the pandemic, the U.S. Drug Enforcement Administration relaxed its guidelines for opioid treatments such as buprenorphine, and it’s allowing doctors to prescribe controlled substances via telemedicine before conducting an in-person evaluation. The Substance Abuse and Mental Health Services Administration, an agency within Health and Human Services, also allowed for opioid use treatments to request exceptions for their clients to take home opioid addiction treatment for up to 28 days, according to agency guidance.
The King County Public Health Department in Washington has recommended that doctors support social distancing by prescribing buprenorphine over the phone and prescribing it for longer periods.
Some “harm reduction” strategies, such as needle-exchange sites, drug-testing kits and managed alcohol programs, were in use before the pandemic, according to the American Addiction Centers, a national network of substance abuse treatment facilities.
Not everyone supports such efforts. Robert McElroy, chief executive officer of the Alpha Project, a San Diego nonprofit that provides housing, substance abuse and hospice programs to the homeless, objects to giving any amount of alcohol or other drugs to people with addictions. His organization runs a 12-week residential treatment program that employs recovering addicts as counselors and staff, and believes recovery requires sobriety – even in quarantine.
“We put people in hotel rooms that we case-manage,” he said. “We’re there to make sure that you’re safe and you’re on the road to recovery.”
But for Kushel at UC San Francisco and other doctors, the necessity of keeping vulnerable people out of hospitals and safe in isolation sheds new light on the debate over harm reduction.
The San Francisco Department of Public Health is providing small amounts of alcohol and nicotine to homeless people with dependencies who are staying in isolation or quarantine sites to curb potentially lethal withdrawal symptoms and encourage them to remain sheltered in place. By providing these substances in measured doses, Kushel said, people are more willing to stay put, and it is much easier to keep them housed. They’re also less likely to abuse alcohol, Malone said, because they’re not in a panic to get it or feel compelled to turn to nonconsumable forms of alcohol, such as hand sanitizer.
“We’ve never been able to make that happen in the U.S.,” Kushel said, despite two decades of advocacy and recognition that alcohol management is a best practice in Canada, Western Europe and Australia. She called the pandemic opportunity “a perfect natural experiment” that researchers are evaluating to see what works and what doesn’t.
A new way of sheltering
Perhaps the most profound lesson of the pandemic, experts said, has been the positive impact of sheltering people in individual rooms.
Shelters have been a crucial resource to serving the homeless in large numbers, but they often are difficult spaces for the homeless, especially those with special needs, said Fay, with Seattle’s downtown emergency center. One of its shelters is on the second floor of a large historical building and contains 238 beds, he said, most of which are bunk beds that are very close together.
“If you’re dealing with anxiety, depression, not to mention a thought disorder like schizophrenia, the symptoms of which can be intense and off-putting and bizarre to many people, you have no choice but to have those play out in public,” Fay said.
The pandemic has made clear that “housing is health care,” a group of leading medical and homeless professionals said in an April 2020 article. Without access to housing, the health care system will continue to be overburdened. They wrote: “Homelessness is extremely dangerous to all who experience it, and has large societal costs.”
Ruth Gonzales, a homeless woman in San Jose, California, said shelters cause her “mind to race,” and the confusion and volume can exacerbate and trigger her PTSD.
Gonzales, 57, has been homeless for the past 11 years, sleeping in parks, school parking lots and under bridges. Living outdoors, she said, has led to physical and verbal assaults. Gonzales said she feels safer now that she’s at the Pacific Motor Inn in San Jose, which was converted into individual housing for high-risk homeless.
She is among thousands of homeless people in California – which has the largest share of the nation’s estimated 600,000 homeless people – who have been housed in hotels and motels as part of Project Roomkey. The state launched the program in early April for homeless people who needed to quarantine or self-isolate. The program funds hotels, motels and emergency shelters, as well as food, security and custodial services, with 75% of the costs reimbursed by the Federal Emergency Management Agency. Phase 2, known as Project Homekey, aims to provide more permanent housing by helping cities, counties and other public entities acquire hotels, motels, apartment buildings, residential care buildings and other facilities for permanent housing.
One of the major benefits of staying in a motel room, Gonzales said, has been access to better food. Living on the street, she said, she wasn’t eating many fruits and vegetables.
Fay said homeless people in shelters have to worry about keeping track of their belongings or finding a bed for the night. If they’re also dealing with mental or physical problems, they might not have the energy to also make sure their diet is healthy.
Eating healthful foods, he said, “is both a result of increased resources being devoted, but also the space in which people are able to receive those resources.”
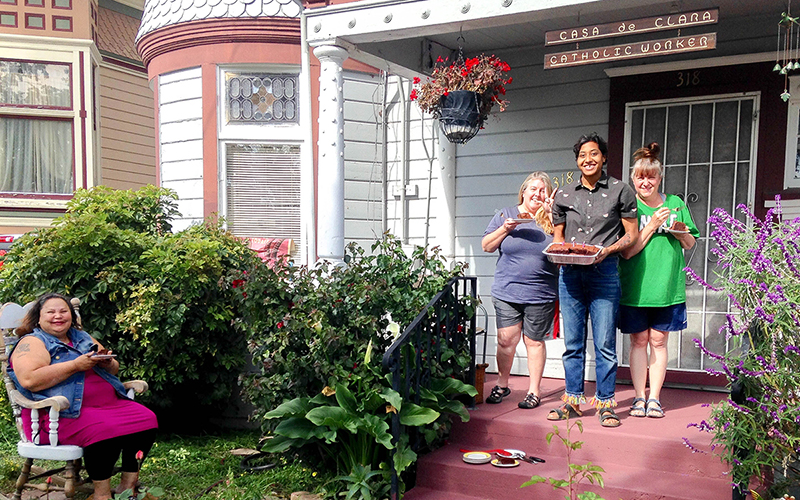
Ruth Gonzales, seated at far left, celebrates her birthday on April 17 with residents of Casa de Clara, a Catholic aid organization in San Jose, California. Social-distancing from her are, from left, Kelly Blake, Artie Evans and Lynn Metz. (Photo courtesy of Casa de Clara)
In Washington, King County also has turned to hotels and motels as a temporary solution to the housing crisis.
The Downtown Emergency Service Center closed three of its large shelters and moved entire operations to hotel settings, Fay said. Residents were moved to the Red Lion, a 225-room hotel leased by the county, and the service center was put in charge of everything from meals to administering services.
Malone, the nonprofit’s executive director, said it increased meal delivery service to the hotel and to the 1,200 apartments the center operates as permanent supportive housing, and staff members are confident they can continue these services after the pandemic ends. There also have been discussions with King County officials about purchasing a hotel for permanent housing, he said.
Providing permanent housing for homeless people is not a new idea, Fay said, but providing it at the scale and speed necessitated by the pandemic was something shelter workers did not think possible.
“I think it is a direct result of COVID-19,” Malone said, “because I don’t think we would be attempting this kind of new way of doing shelter.”
Shelter workers say they have seen dramatic changes in some people who moved from shelters to single-room accommodations.
Shelter life is transitional and chaotic, Fay noted, and “it doesn’t really afford people the time and the space to think about other goals they may have in the same way that moving into an individual hotel room allowed people to do.”
One example was a jogging group formed by some residents of the Red Lion.
“People just decided that they want to start jogging,” Fay said, “which is just unheard of in a congregate shelter setting, not because people didn’t deep down have those goals, they just didn’t have the time and space afforded to them to actually plan to do that kind of work.”
In his 17 years working at the shelter, he said, he’s never seen anything like it.
People in shelters also frequently call 911 if they’re having a medical or mental health crisis or are involved in some interpersonal conflict, Fay said, but when clients moved to the Red Lion, those distress calls dramatically dropped almost overnight.
National nonprofits that have been studying and collecting data on homelessness for decades are not surprised to see how many COVID-19 emergency measures have become silver-lining solutions.
“We know how to solve homelessness,” said Sarah Saadian, vice president of public policy at the National Low Income Housing Coalition. “It’s just about having a political will to invest the resources at the scale necessary. And I’m hoping that this pandemic sheds light on … how important it is to do that.”
This project was supported by the Pulitzer Center and produced by the Howard Center for Investigative Journalism at Arizona State University’s Walter Cronkite School of Journalism and Mass Communication. The Howard Center is an initiative of the Scripps Howard Foundation in honor of the late news industry executive and pioneer Roy W. Howard.
Contact us at [email protected], visit us on Twitter @HowardCenterASU.
