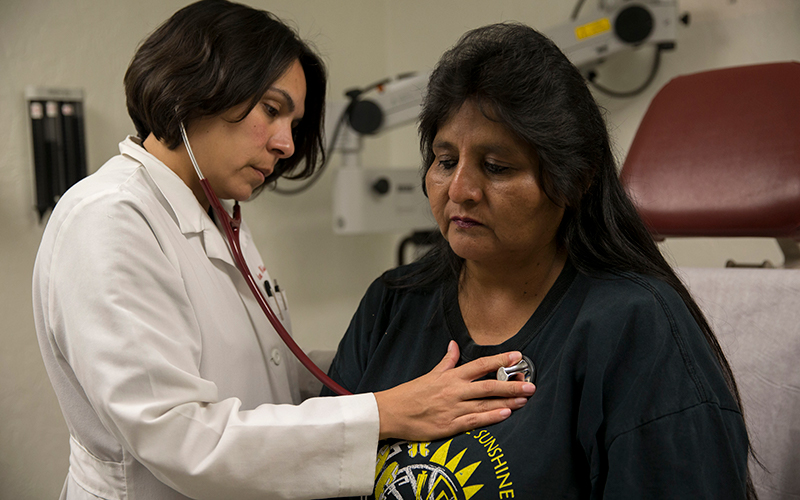
Dr. Dena Wilson examines patient Doris Miguel at the Indian Health Service in Phoenix in this 2017 file photo. The number of IHS patients with health insurance rose in recent years, but still trailed rates in the rest of the nation. (Photo by Megan Bridgeman/Cronkite News)
WASHINGTON – The number of people who showed up at at Indian Health Service facilities with health insurance rose from 64% of patients in 2013 to 78% in 2018, according to a new report from the Government Accountability Office.
The report said growth in coverage was highest in states, like Arizona, that expanded their Medicaid programs as part of the Affordable Care Act, or Obamacare.
Despite the gains, however, the share of people without insurance at the 73 IHS facilities in 2018 was still more than double the national average for health care coverage that year.
Calls to tribal officials and advocates Tuesday seeking comment on the report were not immediately returned. But the GAO report said Native Americans have “long-standing problems accessing needed health care services, and have historically had poorer health than the U.S. general population.”
The report’s authors did not credit Obamacare directly for the improvement in tribal health care, but said that elements of the law helped expand coverage for Native Americans which, in turn, led to a healthier bottom line for facilities serving them.
Revenue at the 73 federally run IHS facilities grew 51 percent from 2013 to 2018, the report said, climbing from $706 million to $1.07 billion. Almost two-thirds of that increase was due to Medicaid payments.
The GAO interviewed representatives from 17 IHS facilities, along with representatives from each of the IHS’ 12 districts. Some of those interviewed said they were able to use the extra funds to offer housing and competitive salaries to doctors, with one clinic reporting a 26 percent drop in turnover.
The biggest change was in the amount of care provided by the Purchased/Referred Care Program. The PRC pays for care of qualifying patients who want or need to seek care outside an IHS facility. The program splits care into levels with more acute and emergency care getting the highest priority, and longer term chronic care getting the lowest.
By expanding the range of care they provided, facilities were able to reduce the need for IHS patients to go private facilities outside the system to seek care. Six years of reduced costs from keeping people within the system let one facility to save enough to build a 23,000-square-foot building to house expanded medical coverage.
The report noted the extra revenues decreased the need for the higher levels of care, because patients were able to use new private insurance or Medicaid benefits to pay for it themselves. This freed up more money, so that the majority of the funds could be allocated for patients needing extended care.
While the report said that states that expanded Medicaid coverage as part of Obamacare saw a higher gain in insurance coverage than those that didn’t – 17% comparted to 8% – the authors said they were not able to provide state-specific gains.
Despite the gains, health insurance coverage still lagged well behind the rest of the country in 2018. The Census Bureau reported last month that about 91% of Americans had coverage in 2018 and a little more than 89 percent of Arizonans did – and both those numbers were down slightly from the year before.
A House Natural Resources subcommittee on tribal affairs last week held a hearing on two bills that would give IHS advance appropriation, funding the agency for two years instead of one. A preliminary report from the National Council on Urban Indian Health described how the partial government shutdown last winter led to layoffs, hiring freezes and delayed care at IHS, and advance appropriations could protect agencies like IHS from whims of Washington politics.